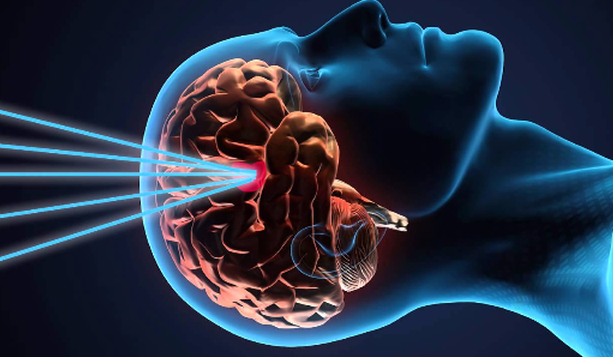
Gamma Knife radiosurgery (GKSRS) is a safe, effective and non-invasive procedure that uses radiation to treat conditions in and around the brain. It is sometimes used as a replacement for conventional surgery, but at other times it may be effective in situations where there is no conventional surgical alternative available. The radiation treatment is delivered with great precision to the target tissue within or around the brain, whilst at the same time minimising any dose to surrounding healthy tissue. The name ‘Gamma Knife’ is in some ways misleading – no knife or cutting implement is actually involved at any stage. The term ‘Gamma Knife’ is intended to convey the idea that this radiation treatment is in some ways delivered as though it were an actual knife because it offers a similar sort of precision and targeting to that offered by actual surgery. It uses radiation in much the same way as a surgeon uses a knife.
If you are unsure if Gamma Knife would be a suitable treatment for your condition or you would like to find out more please contact us. Someone will be in touch to tell you more about the treatment and if it is potentially suitable for you. The multidisciplinary Gamma Knife team meet regularly to discuss new cases and are happy to review your scans. There is no cost for this service. The team includes a neurosurgeon, radiation oncologists, medical physicist and nurses. Once your case has been discussed we will be in contact shortly afterwards to let you know if Gamma Knife is an option for you or if not we may be able to advise on other treatments. It can be a very valuable second opinion free of charge.
Radiation damages the DNA in the cells of a tumour or other abnormality being treated, such that the cells that make up the targeted tissue can no longer reproduce. Eventually, when these cells come to the end of their natural lifespan, they find that they are unable to reproduce and replace themselves because the DNA essential to this process is no longer functioning properly. Some lesions which are very inactive in terms of cell function may take up to 2 or 3 years or more to respond to treatment -this is typically the case for instance with blood vessels and arterio-venous malformations (AVM) which usually resolve over this sort of time period.
Yes – in terms of the risk of damage to the tissue around the target area. GKSRS risks can nearly always be brought down to very low levels – one of the more common reasons for recommending GKSRS is that the overall risk compared to open surgery is frequently much lower. This is sometimes so much the case that the surgical alternative may actually carry a higher overall risk than that of the condition being treated, thereby rendering it effectively inoperable other than by radiosurgery. The precise nature and magnitude of any risk will vary with the size, nature and position of the lesion being treated. You should ask your treating doctor to elaborate on the details of this with respect to your own individual situation – they will be more than happy to give you a very full explanation of all that is involved. As with any form of surgical or radiation treatment, there will always be some small risk attached and this can never be reduced to zero.
Serious complications of GKSRS are really very unusual. Minor side effects, which generally resolve within a few hours, are sometimes seen and do not usually present the patient (or the doctor) with a significant problem. It is fair to say that the large majority of patients suffer no side effects whatsoever, apart perhaps from a feeling of being a bit tired and ‘washed out’ at the end of a busy day’s treatment! We tend to think of complications in terms of those which may occur early i.e. soon after treatment, and those which can occur at a later stage, some weeks or months following GKSRS:
Common Early Complications
- Some local discomfort of the scalp relating to the pin sites which are used to fix the frame – resolves within a few hours, almost certainly by the following morning.
- Numbness of the scalp around pin sites may occur which resolve over a day or two.
- A headache – again usually mild, resolving rapidly.
- Mild nausea.
Benefits Include:
- The risks of infection, haemorrhage and spinal fluid leakage are eliminated, as is the scarring and potential disfigurement that results from conventional neurosurgery.
- The small risk associated with general anaesthesia is also eliminated. A mild sedative is occasionally used.
- GKSRS is a day procedure except in occasional circumstances.
- GKSRS sometimes can be used in conjunction with conventional surgery, usually taking the place of the more risky component of the latter. In other words, where conventional surgery is absolutely required, its risk can be reduced by partially substituting GKSRS as a ”boost” to perform the final part of the job.
- An individual who might be a relatively high-risk candidate for conventional surgery may be a much safer candidate for GKSRS.
- Unlike whole brain radiotherapy GKSRS is directed very specifically at the target. This spares most of the adjacent normal brain tissue from exposure to unnecessary excess radiation.
- “Fractionation” is not required – unlike radiotherapy (such as Linac and SRS which may require fractionation) which is often delivered in many fractions over several weeks, GKSRS can nearly always be delivered as a single treatment over the course of less than a day. Multiple hospital visits are therefore avoided.
- As a day case treatment, GKSRS offers the prospect of return to work, driving, and other normal social activities within a few days in the vast majority of cases. This is frequently as soon as the day following treatment.
- Established effectiveness over 40 years of experience worldwide, with a very low rate of complications
The stereotactic frame is fitted under local anaesthesia. This involves the administration of 4 small injections around the circumference of the head, in order to numb the sites where the 4 pins are to be used to secure the frame. The experience of these is the same as when visiting the dentist for the purpose of having a tooth put to sleep for filling. The same local anaesthetic drug is used in both instances. Very quickly, after a brief stinging sensation, these areas will go numb. The frame is then attached. As the pins are secured you will feel a strange “pressure” sensation which quite soon passes. The whole procedure takes about 5 – 10 minutes, and after the frame is fitted you will gradually get used to the sensation. After a short while, you will no longer feel this, and you will almost forget that the frame is there at all! Frame fitting involves a small degree of discomfort, but most patients tolerate it remarkably well and tend to comment that it was much preferable to the idea of having a major surgical procedure performed. At the end of the procedure, the frame is removed. This only takes a minute or two and is really not at all traumatic. Some patients experience headaches after frame removal which can be treated with simple pain relief.
No. All radiation stays within the treatment room. The Gamma rays used in the treatment do not remain in the body.
In the postoperative period, some tumours may swell a little as a result of being injured by a dose of radiation. This may show as a slight increase in apparent size of a tumour as assessed by MRI or CT scanning at about 6-9 months post-treatment. This appearance must not be misinterpreted as tumour growth. It is self-limiting, and will soon be followed by reduction back to original size, or even smaller. If this temporary swelling (which is actually indicative that the treatment is starting to work) causes any symptoms, then a short course of steroids or other medication is sometimes used to treat the swelling.
The vast majority of patients have no risk whatsoever of losing any hair at all. Furthermore, even in those few cases where hair loss is a possibility, such hair loss will never involve the entire scalp – as typically happens with whole brain radiotherapy. Only a small number of patients will have tumours sufficiently close to the scalp to carry the risk of any hair loss at all. If a lesion to be treated is very close to the inside of the skull, it is possible that enough radiation will be delivered to the scalp such that a patch of hair the size of a 10 or 20 cent coin may be lost. This hair usually grows back, though it may be a little lighter in colour and finer in texture than previously.
Theoretically yes – all forms of radiation can in principle cause tumour formation – but instances of this actually happening are so rare that there is no direct scientific proof that it has been caused by treatment. There are some individuals (with rare conditions) who are at risk from developing further tumours because of their underlying condition, and very occasionally (perhaps a dozen times out of tens of thousands of patients over several decades), such new tumour formation has been reported. Based on existing experience, the incidence of radiation caused tumours is extremely low, much less than the risk of a complication arising from a general anaesthetic for example.
Most patients feel just as well as they did at the beginning of the day. Some tiredness is quite common, especially if the treatment has occupied most of the day. A little discomfort at the pin sites and a mild headache are also quite common – this may persist for up to a day or two. Mild nausea may also occur during the first 48 hours following treatment. Mild anti-nausea and headache medication are routinely prescribed for patients who may require it. Patients are observed for one to two hours post-treatment.
As soon as you feel well enough. There is no reason why you should not go back to work the following day – some patients have even been known to return to work later the same day, but you should not feel pressured to return to work too quickly. It is fair to say that most people return to work within less than a week.
Again, as soon as you feel well enough. There is no reason why you could not travel the following day, or even sometime later on the actual day of treatment. Any driving restrictions already in place will continue to apply.
You will see a Neurosurgeon and/or Radiation Oncologist approximately 4 to 6 weeks post-treatment, just to check that everything is ok. Depending on the condition treated, they will arrange for follow-up scans to be performed usually at 3 months post-treatment.
Gamma Knife radiosurgery is used to treat certain conditions of the brain, many of which could only be treated by open surgery had this option not become available. At the Gamma Knife Center, our expert neurosurgeons and radiation oncologists most often use the Leksell Gamma Knife Icon to treat the following brain conditions:
Primary brain tumours, in particular:
- Acoustic neuroma/Vestibular Schwannoma
- Pituitary tumour
- Craniopharyngioma
- Glioma
- Meningioma
- Hemangioblastoma
- Glomus jugulare tumour
Additionally:
- Chordoma
- Pediatric brain tumours
- Arteriovenous malformation
- Trigeminal neuralgia
- Essential tremor
- Epilepsy
- Obsessive-compulsive disorder
Other conditions may also respond to Gamma Knife radiosurgery. This may be the procedure of choice when a brain lesion cannot be reached by conventional surgical techniques. Gamma Knife may also be used in lieu of operations that require craniotomy for those patients who must avoid open surgery.
Because the therapeutic effects of a Gamma Knife procedure occur over time, it may not be suitable for individuals whose condition requires more immediate therapy.
Gamma Knife radiosurgery can be used to treat children and adults.
At Gamma Knife Center, the treatment team typically includes a neurosurgeon, a radiation oncologist, a radiation therapist and a registered nurse. In addition, a medical physicist calculates the precise beam placement and number of exposures necessary to obtain the radiation dose that is prescribed by the radiation oncologist. (Your treatment team may include other healthcare professionals in addition to, or in place of, those listed here.)
A Gamma Knife procedure may be performed on an outpatient basis or as part of your stay in a hospital. Procedures may vary slightly depending on your condition.
Before the procedure begins, you may be asked to remove any clothing, jewellery, hairpins, dentures or other objects that may interfere, and you will be given a gown to wear. An intravenous (IV) line may be started in your hand or arm in order to supply you with medications and/or fluids.
Next, the head is prepared for placement of a box-shaped head frame or custom-made face mask. No shaving is required for either method. Which method is used depends on the individual condition and diagnosis of the patient. Frames confer maximum precision, necessary for working with trigeminal neuralgia, essential tremor, epilepsy and obsessive-compulsive disorder. Face masks, which may be more comfortable, also ensure an extremely high degree of accuracy. The frameless face mask also enables treatment of larger tumours over a series of days usually on an outpatient basis. The frequency and amount of treatments required will be determined by the Gamma Knife team.
If a head frame is used the head frame is attached to the head and will prevent the head from moving during the procedure. This technique is also called frame-based radiosurgery.
If a face mask is used, a thermoplastic mask will be placed and then moulded over your face for a customized fit. The mask has an opening for your nose and you will be able to breathe comfortably while wearing it. The mask is then contoured to fit your face perfectly and will have a snug, tight fit, minimizing head movement during the procedure. It will take about 10 minutes or less for the mask to harden, forming a custom face mask. Although tight, the face mask is comfortable to wear throughout the procedure. This technique is also called frameless radiosurgery.
You may receive a mild sedative to help you relax prior to a frame or frameless procedure.
After the head frame or face mask is attached, you will undergo brain imaging so that the location of the brain lesion can be precisely identified. The brain imaging procedure may be a computed tomography (CT) scan, a magnetic resonance imaging (MRI) scan or a cerebral angiogram.
After the brain imaging has been completed, you will be allowed to rest and relax while the treatment team completes your treatment plan. Determining your treatment plan can take between 30 and 90 minutes. To make your treatment plan, the team will combine the results of the imaging scan with other information to determine optimal dosage and number of exposures. The team will input specific instructions to the computer system on where to focus the gamma rays, ensuring pinpoint precision and accuracy.
When your treatment plan is ready, you will be taken into the room where the Leksell Gamma Knife Icon is located. You will lie down on a sliding table, with your head pointing toward the machine. The table will then slowly slide you into the wide opening of the Gamma Knife unit.
During the entire treatment, you will be monitored by the Gamma Knife team via live video feed. You will have an intercom available to communicate with the team. They will be able to hear and communicate with you at all times.
The Icon machine is silent and you will not feel or hear anything during the procedure. The team will continuously monitor your head placement and radiation dosage. The head frame or face mask will keep your head in alignment. The Leskell Gamma Knife Icon has a safety feature that blocks radiation if movement occurs.
The number of treatment sessions will depend on your specific diagnosis. You may be inside the Gamma Knife unit as briefly as 15 minutes, or up to a few hours; the duration will depend on the treatment plan designed for you.
After the treatment session is over, the treatment table will slide out of the Gamma Knife machine.
The head frame or face mask will be removed. You will then be briefly monitored by the nursing team prior to discharge.
Although Gamma Knife radiosurgery is less invasive than traditional open surgery, there are some possible side effects and risks.
Radiation therapy is not recommended to women who are pregnant. Women of childbearing age may need to provide a urine sample prior to Gamma Knife treatment to ensure they are not pregnant.
Other side effects may include cerebral oedema, headache, nausea, numbness or weakness in the face, loss of balance, vision problems, hair loss near the treated area (the hair loss is usually temporary) and seizures. Medication can be used for many of these side effects. Your physician will explain possible side effects before the procedure and manage any side effects after the procedure, should they occur.
There may be other risks, depending on your specific medical condition. Be sure to discuss any concerns with your physician prior to the procedure.
Your physician will explain the procedure to you and offer you the opportunity to ask questions. You will be asked to sign a consent form to give your medical team for permission to undertake the procedure. Please read the form carefully and ask questions if anything is not clear.
Be sure to tell your physician if you are sensitive or allergic to any medications, latex, tape, contrast dyes or iodine. Also inform your physician of all medications, both prescription and over-the-counter, and all supplements, including herbs or vitamins, that you are taking.
If you are taking any anticoagulant medications, aspirin or other medications that affect blood clotting, it may be necessary for you to stop these medications temporarily before undergoing the procedure.
Tell your physician if you have an implant, such as a pacemaker and/or implantable defibrillator, artificial heart valve, surgical clips for a brain aneurysm, implanted medications pump, chemotherapy port, nerve stimulators, eye or ear implants, stents, coils or filters and shunts.
The morning of the procedure, eat a light breakfast at home and wear loose, comfortable clothing when you arrive. Do not wear jewellery or makeup.
Be sure to arrange transportation because you will not be permitted to drive yourself home after the procedure.
The Gamma Knife procedure is generally performed on an outpatient basis, so you will go home at the end of the day.
No, you will not need to take any special medications for the procedure. If you feel some discomfort after the procedure, such as a headache or nausea, you will be given medication for relief.
Once you are home, you can resume most of your normal activities. You can resume exercise and other forms of strenuous activity about 18 to 24 hours after the procedure unless your physician instructs you differently.
After the procedure, you will receive a follow-up call from the Gamma Knife nursing team. Follow-up appointments will be discussed with your neurosurgeon and possibly other team members. During these appointments, imaging studies may be ordered to monitor the treated lesion and determine the effect radiation had on it. Gamma Knife radiosurgery may take weeks, months or years to work.
If you experience any of the following, call your physician or emergency depending on the severity of symptoms:
- A severe headache that is not relieved by medication
- Any weakness, numbness or vision problems that are new or have become worse than they were before the procedure
- Seizures
- Unable to tolerate liquids and persistent vomiting
- Temperature greater than 100.4 degrees Fahrenheit over a 24 hour our period unrelieved by medications.
Usually, patients do not have any long-term limitations as a result of Gamma Knife radiosurgery. Some possibility of long-term limitations may exist as a result of the underlying condition treated. Please ask your doctor about your own situation.
The Gamma Knife is not actually a knife at all. It is a stereotactic radiosurgical device that non-invasively treats malignant and benign brain tumours, vascular malformations and trigeminal neuralgia in a single patient visit. Patients are treated on an outpatient basis or may require an overnight hospital stay.
Utilizing advanced diagnostic imaging and three-dimensional treatment planning software, Gamma Knife delivers 192 precisely focused beams of gamma radiation to small targets inside the brain. Radiation is only delivered at a single, finely focused point where all 192 beams converge to treat the diseased tissue, while the nearby healthy tissue is spared.
Gamma Knife Perfexion treatment has many benefits. It is bloodless, virtually painless, does not result in hair loss and has a rapid return to pre-treatment activities. Gamma Knife treatment also has excellent, well-documented clinical outcomes for a variety of brain diseases and disorders.
There are also several benefits of having Gamma Knife radiosurgery versus other forms of radiation or surgery. The benefits of Gamma Knife Perfexion treatment differs from conventional radiation therapy of the brain because it is only directed to targeted areas and spares unnecessary treatment of adjacent, normal brain tissue. Only a one-day treatment is required rather than many treatments over several weeks, and the treatment often can be repeated if necessary.
Gamma Knife treatment can also replace brain surgery in some patients with brain tumours, vascular malformations and facial pain. An individual who would be at risk for complications from conventional surgery may be a candidate for Gamma Knife radiosurgery. Gamma Knife treatment can be used when prior surgery or radiation therapy has failed to control the disease process. It can also be used in conjunction with conventional surgery in previously inoperable cases, other forms of radiation therapy and chemotherapy.
Gamma Knife radiosurgery is especially valuable for patients whose neurological disorders require a difficult surgical approach or may be impossible to treat using conventional neurosurgical techniques. Patients of advanced age or in poor medical condition can be at an unacceptably high risk for anaesthesia and conventional surgery, making Gamma Knife treatment an ideal solution. Gamma Knife technology also is highly beneficial for patients whose lesions are situated in an inaccessible or functionally critical area within the brain. In addition, the treatment can be used as an adjunct to the care of a patient who has undergone conventional brain surgery, interventional neuroradiology or conventional radiation therapy or chemotherapy.
Conditions for which the Gamma Knife is considered are:
- Malignant tumours such as metastases (cancer that has spread to the brain) and malignant gliomas
- Benign tumours such as meningiomas, acoustic neuromas (vestibular schwannomas), pituitary tumours and low-grade glioma and skull-based tumours
- Vascular malformations such as arteriovenous malformations (AVMs) and cavernous angiomas (cavernous malformations)
- Functional disorders such as trigeminal neuralgia
Most patients are referred to the Gamma Knife program by their doctors. However, some make self-referrals. The Gamma Knife team reviews each patient’s records to determine if Gamma Knife treatment would be advantageous.
The following information is considered:
- Medical and surgical history
- Clinical examinations
- Imaging studies, such as MRI, CT and/or PET scans
The Gamma Knife’s success rate is impressive. Supported by more than two decades of clinical research, this neurosurgical tool has met with unprecedented results. Clinical applications continue to grow, and its many benefits as a non-invasive treatment modality continue to make it the treatment of choice for certain clinical conditions.
Once a patient’s condition is reviewed by our multidisciplinary team and Gamma Knife treatment is deemed appropriate, the patient will be scheduled for a treatment day. On the day of treatment, there are several steps that take place. First, a lightweight frame is attached to the patient’s head. Local anaesthesia is used before the frame is secured in place. The patient then has an MRI or CT imaging study, or in the case of an arteriovenous malformation, angiography may be needed in order to precisely locate the diseased area. Data from the imaging study is transferred into the treatment planning computer. While the patient rests, the treatment team (a neurosurgeon, radiation oncologist and physicist) uses advanced software to determine the treatment plan. This takes one or two hours to complete, depending on the complexity and location of the disease. When the individual treatment plan is completed, the patient is placed on the Gamma Knife couch and precisely positioned. The patient has then moved automatically, head first into the machine, and treatment begins. Treatment typically lasts from 15 minutes to an hour or more, during which time the patient feels nothing unusual.
Actual treatment time varies based on the condition being treated and its location. Following treatment, the patient is automatically moved out of the machine, and the head frame is removed.
During the actual procedure, the patient does not see or feel the radiation during treatment. Before the treatment takes place, patients typically feel slight discomfort from the local anaesthetic used prior to head frame placement, and have reported feeling pressure for a short time while the pins are inserted to fixate the head frame, but no pain.
The patient remains conscious throughout the entire procedure and may communicate with the treatment team.
No, the head is not shaved. In rare cases, the treatment may cause some hair loss.
When the treatment is finished, the head frame will be removed. Sometimes there is a little bleeding from where the pins were attached to the head. In this case, gauze and pressure will be applied to stop the bleeding and keep the area clean. A temporary head dressing is placed to keep the pin sites clean. It is recommended that the patient take it easy over the next 12 to 24 hours. Pre-Gamma Knife activities can be resumed within a few days.
The Gamma Knife allows non-invasive brain surgery to be performed with extreme precision while sparing healthy tissues surrounding the targeted treatment area. Also, because neither a surgical incision nor general anaesthesia is required, the risks usually involved with open brain surgery, such as haemorrhage or infection, may be reduced. Hospitalization is rarely required and recovery time is minimal. While individual patient outcomes may vary, patients may resume their normal pre-surgery lifestyle within a few days.
The effects of Gamma Knife radiosurgery occur over several days to several years, depending on the type of medical condition treated. The radiation alters the DNA of a tumour or lesion being treated so that the cells no longer reproduce, eventually rendering the lesion inert. Some abnormalities dissolve gradually, eventually disappearing. Others simply exhibit no further growth. The effectiveness of the treatment is monitored by MRI scans at regular intervals. The goal of radiosurgery is tumour control, which is defined as a stable tumour size or tumour shrinkage.
Early complications may include:
- Common side effects – local pain and swelling in the scalp and headache
- Rare complications – skin reddening and irritation, nausea and seizure
Delayed complications may include:
- Uncommon complications – local loss of hair in superficial lesions, local brain swelling in the treatment site and local tissue necrosis in the treatment site
- Rare complications – visual loss (dependent on diagnosis and areas treated) and hearing loss (dependent on diagnosis and areas treated)
Within a few days. The only restrictions you will have are the same you had prior to your treatment.
Cost studies have shown Gamma Knife radiosurgery to be less expensive than conventional neurosurgery because it eliminates lengthy post-surgical hospital stays, expensive medication and potentially months of rehabilitation. Importantly, there are virtually no post-surgical disability and convalescent costs with this procedure.
?Yes, Gamma Knife radiosurgery is covered by most health insurance companies.